Put your health in safe hands with microsurgical varicocele surgery technology.
Assoc.. Prof. Dr. Muhsin BALABAN graduated from Marmara University Faculty of Medicine (English) and completed his residency in Urology at Kartal Dr. Lütfi Kırdar Training and Research Hospital.
He spent 3 months in the United States of America to increase his knowledge and experience at Celveland Clinic, Albert Einstein University and Memorial Sloan-Kettering hospitals respectively.
Since 2014, he has been working intensively on Male Reproductive Health, Microscopic Varicocele surgery, MicroTESE, Sperm enhancement treatments, Azoospermia, Erectile Dysfunction and Treatments. In 2018, he started his academic studies as a lecturer at Biruni Faculty of Medicine and Beykent University. In 2019, he received 1-month intensive training on Azoospermia and Varicocele surgery at ProCrea Infertility Center in Switzerland and San Carlo Clinic of Milan University in Italy with Prof. Dr. Giovanna Maria Colpi.
He has been successfully performing varicocele surgeries using microsurgical technique for 10 years. For the last 5 years, he has been performing ONLY microscopic varicocele surgery and microTESE operations upon intense demand from Turkey and abroad.











It was established by Assoc. Prof. Dr. Muhsin BALABAN in 2019 exclusively for diagnoses and treatments related to male reproductive health. Solutions are offered at international standards with the latest technological equipment for the treatment of men with low sperm count, azoospermia or after failed IVF attempts and especially for the diagnosis and treatment of VARICOCEL disease.
In addition to microscopic surgery in varicocele surgery, the use of 1.5 mm intraoperative doppler technology in addition to microscopic surgery shows the arterial structure feeding the testicle more clearly and is a more careful operation.
Assoc. Prof. Dr. Muhsin Balaban started to perform all his surgeries using intraoperative doppler after 2018. Likewise, he contributed to the development of the technique of cutting out the enlarged vessels to reduce recurrence and provide rapid improvement in testicular swelling. He explained these innovations and experiences in varicocele surgery to his colleagues in Turkey with live video at the Andrology congress.
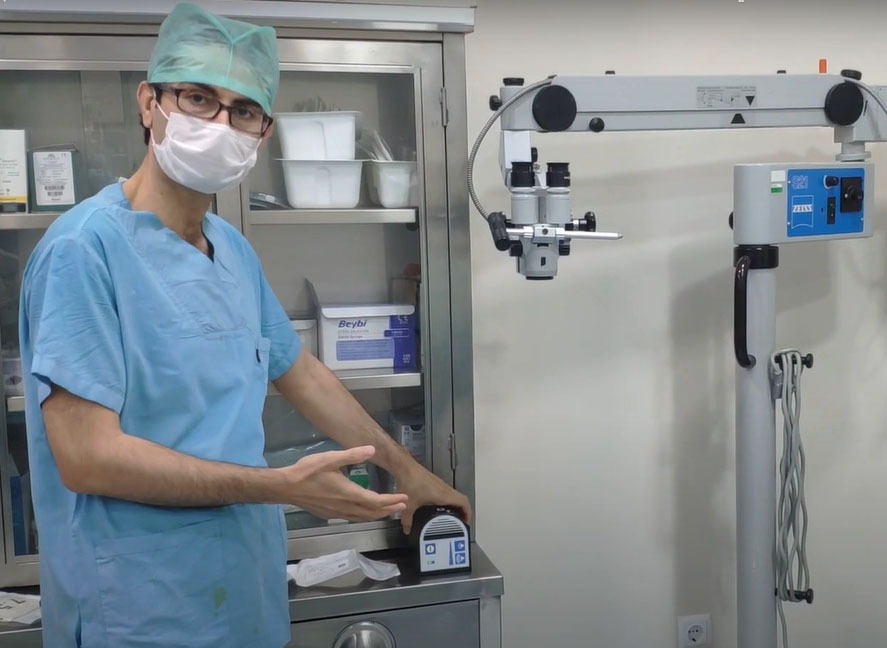
With this technology, very sensitive arteries are protected and the margin for error is almost completely eliminated. It is more successful than other techniques. In the United States this Doppler Technology is very widely used. Since 2018, I have been using this technology in all my surgeries.
Varicocele is an abnormal enlargement of the veins around the testicle.
Veins are the vessels in the body that bring blood back to the heart. Normally there are valves in the veins that keep the blood moving in the right direction. However, because the valves in the testicular veins are damaged and do not function properly, gravity causes the blood to pool around the testicle. This clinical picture is more common on the left side.
Varicocele is common in men and indeed 15% of adult men have varicocele. But most of the time it does not harm the patient.
Varicocele can cause 3 different basic problems;
1-It may cause infertility by impairing sperm quality
2-It may affect the production of testosterone from the testis
3-It may cause pain and a feeling of fullness in the testicle
To treat varicocele, at least one of the 3 reasons above must be present. In some cases, varicocele can cause azoospermia (no sperm in semen).
Because varicocele is so common in men and often goes undiagnosed, most patients do not experience any hormonal problems, testicular pain or reproductive problems.
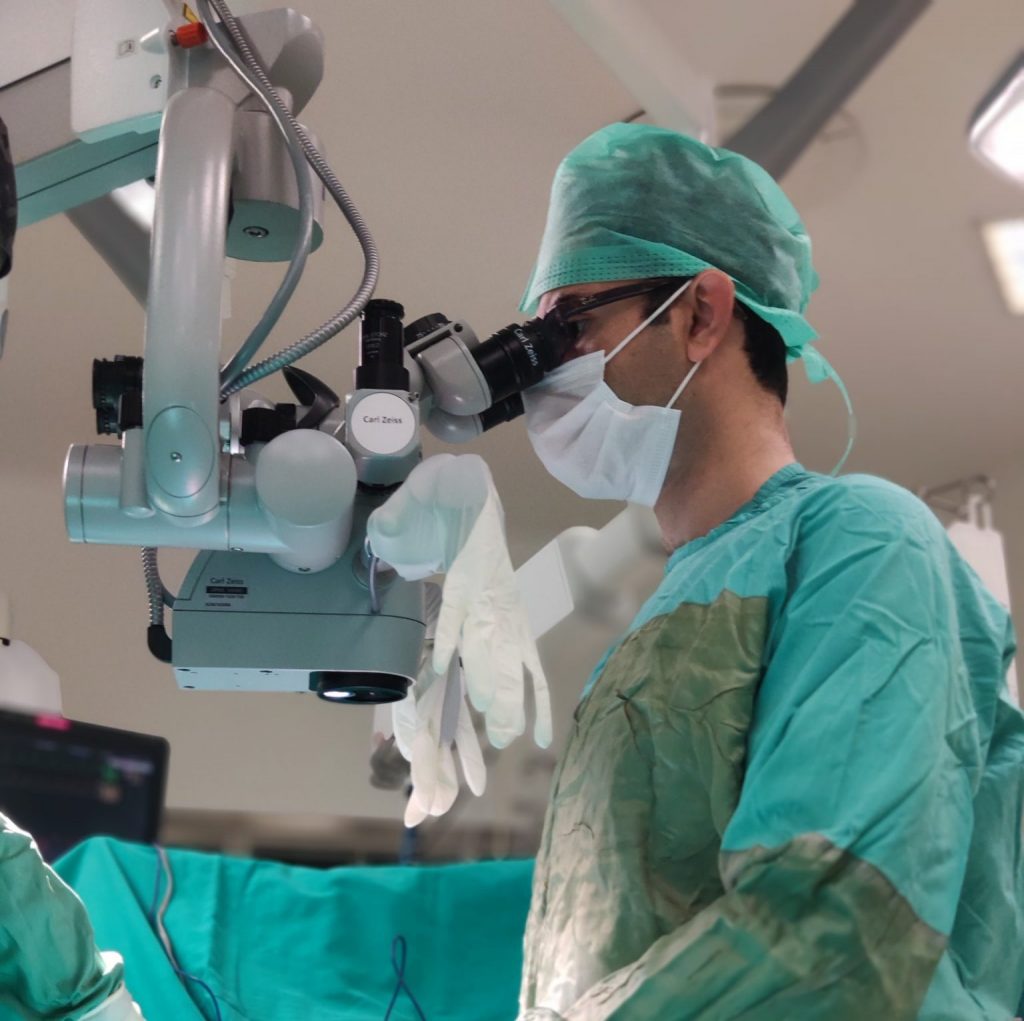
The surgery can be performed under general or spinal anesthesia. Through a 2 cm incision in the groin area, the spermatic cord is found and suspended. The veins are identified, ligated and cut. Meanwhile, important structures leading to the testicle (vas deferens, testicular artery and testicular lymphatic vessels) are preserved.
 Since the muscles are not cut in this method, there is less pain after surgery and the risk of postoperative inguinal hernia is reduced. By protecting the lymphatics with the microscope, the risk of fluid accumulation around the testicle (hydrocele) after surgery is greatly reduced.
Since the muscles are not cut in this method, there is less pain after surgery and the risk of postoperative inguinal hernia is reduced. By protecting the lymphatics with the microscope, the risk of fluid accumulation around the testicle (hydrocele) after surgery is greatly reduced.

Potential risks after surgery include recurrence or persistence of varicocele, testicular tenderness and infection. Although there is a risk of hydrocele (fluid accumulation around the testicle), this risk is greatly reduced after varicocele surgery using a microscope. Very, very rarely, if the artery leading to the testicle is injured, in less experienced hands, there may be a risk of losing the testicle.

After at least 1 year follow-up of 540 male patients who were unable to have children and diagnosed with significant varicocele after microscopic varicocele surgery;
 Data from a recent study showed that up to 10% of patients with advanced varicocele and concomitant azoospermia spontaneously recovered after varicocele surgery.
Data from a recent study showed that up to 10% of patients with advanced varicocele and concomitant azoospermia spontaneously recovered after varicocele surgery.

In recent years it has been shown that varicocele damages sperm DNA and is responsible for unexplained infertility or recurrent miscarriages. Therefore, in such cases, each case should be evaluated in detail and if necessary, varicocele disease should be corrected to improve sperm quality even if the sperm count is normal.
CALL US
Send us your e-mail address and we will send you news from our clinic.